Blog
The Importance of CPR Certification in Tampa: Saving Lives Made Easy
Cardiopulmonary resuscitation (CPR) certification is a crucial qualification that equips individuals with life-saving skills in emergency situations. In this blog post, we will delve into the significance of CPR certification, highlighting its immediate response benefits, increased survival rates, and the confidence and preparedness it instills in individuals. With CPR training, individuals in Tampa can become empowered to save lives effortlessly.
The Significance of CPR Certification
During a cardiac emergency, time is of the essence. CPR certification ensures that individuals are prepared to respond promptly and appropriately in such situations. By initiating CPR immediately, trained individuals can maintain blood flow and oxygenation to vital organs until professional medical help arrives, significantly increasing the chances of survival for the victim. Statistics reveal that the survival rates of cardiac arrest victims are significantly higher when CPR is initiated early. CPR certification equips individuals with the knowledge and skills to perform effective chest compressions and rescue breaths, enabling them to sustain the vital functions of the body until advanced medical assistance is available. By obtaining CPR certification, you become a vital link in the chain of survival, potentially saving a life in your community.
CPR certification not only imparts life-saving skills but also instills confidence and preparedness in individuals. Knowing that you possess the ability to intervene in a critical situation can make a significant difference in your response. With proper training, individuals can remain composed and act confidently, providing the necessary support and care until professional help arrives.
CPR Training: A Life-Saving Skillset
CPR training provides individuals with a comprehensive understanding of basic life support techniques. Participants learn how to assess a victim’s condition, perform chest compressions, deliver rescue breaths, and manage an obstructed airway. These fundamental skills are essential in maintaining blood circulation and oxygenation during cardiac emergencies. CPR training emphasizes the importance of early intervention.
Participants learn to recognize the signs of cardiac arrest, activate the emergency response system, and initiate CPR promptly. By understanding the critical role of early intervention, individuals can take immediate action, potentially saving a life before professional help arrives. Automated external defibrillators (AEDs) play a crucial role in cardiac emergencies. CPR training provides individuals with the knowledge and confidence to use an AED effectively.
Participants learn how to recognize a cardiac rhythm that requires defibrillation, apply the AED pads correctly, and deliver shocks if necessary. By incorporating AED training into CPR certification, individuals are prepared to respond comprehensively to cardiac emergencies.
The Benefits of CPR Certification in Tampa
By obtaining CPR certification, individuals contribute to building a safer community in Tampa. The more people trained in CPR, the higher the chances of a quick and effective response during cardiac emergencies. Each certified individual becomes an asset to their community, capable of saving lives and making a significant impact in times of crisis.
CPR certification is highly valued in various professions. Many healthcare, educational, and childcare facilities require employees to hold CPR certification. By obtaining this qualification, you enhance your employability and open doors to career opportunities that prioritize life-saving skills. Additionally, employers recognize CPR certification as a demonstration of responsibility, dedication, and the ability to handle emergencies efficiently.
CPR certification empowers individuals with the ability to make a difference. Knowing that you possess the skills to save a life can be empowering and gratifying. By becoming CPR certified, you join a community of compassionate individuals dedicated to helping others and creating a safer environment.
CPR Training Sites in Tampa: Why Choose CPR Tampa
CPR Classes Tampa offers accredited training programs recognized by the American Heart Association (AHA). Accreditation ensures that the training adheres to industry standards and equips participants with up-to-date, evidence-based techniques.
CPR Classes Tampa boasts experienced and qualified instructors who possess the necessary certifications and expertise to deliver comprehensive training. These instructors ensure that participants receive a top-quality education and hands-on practice, enabling them to become competent and confident in CPR techniques.
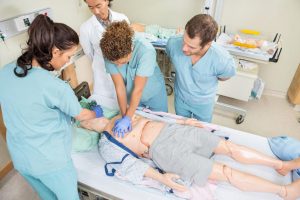
CPR Tampa provides hands-on training and simulations that replicate real-life scenarios. Through practical exercises, participants gain valuable experience and develop the muscle memory required to perform CPR effectively. By simulating emergency situations, CPR Tampa ensures that individuals are prepared to respond appropriately and confidently when faced with a cardiac emergency.
CPR certification in Tampa is a vital qualification that saves lives and empowers individuals in Tampa. By acquiring CPR skills, individuals can respond immediately, increase survival rates, and provide critical support during cardiac emergencies. CPR Classes Tampa offers accredited training programs, experienced instructors, and hands-on practice to ensure participants receive a comprehensive education. Join the ranks of CPR-certified individuals in Tampa and make a difference in your community. With CPR certification, saving lives becomes easy, and you become an invaluable asset in times of crisis.



[grw id=”11782″]
Be Prepared to Save a Life: Top Reasons to Enroll in CPR Training
 Imagine finding yourself in a situation where someone suddenly collapses and stops breathing. Would you know what to do? Being prepared to save a life is a crucial skill that everyone should possess. In emergencies, every second counts, and an immediate response can make all the difference. That’s where CPR training comes in. It equips individuals with the knowledge and skills needed to provide life-saving assistance. In this blog post, we will explore the significance of CPR training and the top reasons why you should enroll in a CPR training program. Life is unpredictable, and emergencies can happen at any time. Whether it’s a cardiac arrest, drowning, or choking incident, knowing how to perform CPR can be the difference between life and death. Being prepared to save a life means having the confidence and ability to take immediate action when faced with a medical emergency. CPR stands for Cardiopulmonary Resuscitation, a technique used to manually maintain blood circulation and provide oxygen to a person’s brain and vital organs during cardiac arrest or respiratory failure. CPR training courses are designed to teach individuals the proper techniques and procedures for performing CPR effectively. Let’s explore the significance of CPR training in more detail.
Imagine finding yourself in a situation where someone suddenly collapses and stops breathing. Would you know what to do? Being prepared to save a life is a crucial skill that everyone should possess. In emergencies, every second counts, and an immediate response can make all the difference. That’s where CPR training comes in. It equips individuals with the knowledge and skills needed to provide life-saving assistance. In this blog post, we will explore the significance of CPR training and the top reasons why you should enroll in a CPR training program. Life is unpredictable, and emergencies can happen at any time. Whether it’s a cardiac arrest, drowning, or choking incident, knowing how to perform CPR can be the difference between life and death. Being prepared to save a life means having the confidence and ability to take immediate action when faced with a medical emergency. CPR stands for Cardiopulmonary Resuscitation, a technique used to manually maintain blood circulation and provide oxygen to a person’s brain and vital organs during cardiac arrest or respiratory failure. CPR training courses are designed to teach individuals the proper techniques and procedures for performing CPR effectively. Let’s explore the significance of CPR training in more detail.
The Significance of CPR Training
In emergency situations, time is of the essence. The first few minutes following a cardiac arrest are critical, and the chances of survival decrease with each passing minute. CPR training emphasizes the importance of immediate response, teaching individuals how to recognize the signs of cardiac arrest and act promptly to provide life-saving interventions. Studies have shown that early CPR can significantly increase the chances of survival for individuals experiencing cardiac arrest. By performing CPR, trained individuals can help maintain blood circulation until professional medical help arrives. CPR training equips individuals with the skills to effectively perform chest compressions and rescue breaths, maximizing the chances of survival for someone in need.
Top Reasons to Enroll in CPR Training
- Ensuring the safety of loved ones
Having CPR knowledge within a household is invaluable. Cardiac emergencies can occur within the family, and knowing how to perform CPR can mean saving the life of a loved one. By enrolling in CPR training, you can ensure the safety and well-being of your family members. By becoming CPR certified, you become a lifeline for your family and friends. In the event of a cardiac emergency, you will have the skills and confidence to provide immediate assistance until professional help arrives. This ability can make all the difference in saving a loved one’s life.
- Being a valuable asset in the workplace
Many employers recognize the importance of having employees trained in CPR. By obtaining CPR certification, you enhance your employability and stand out among other job applicants. CPR training demonstrates your commitment to safety and your ability to handle emergency situations, making you a valuable asset to any workplace. In the workplace, emergencies can occur, and quick action is vital. By enrolling in CPR training, you contribute to creating a safer work environment for your colleagues. Your knowledge and skills can make a difference in critical situations, providing immediate assistance to a coworker in need.
- Empowering oneself to take action in public settings
Medical emergencies can happen anywhere, whether you’re at a park, shopping mall, or attending a public event. CPR training empowers you to take action in these public settings. You become equipped with the skills to recognize emergencies, initiate CPR, and potentially save lives. Having the ability to assist in emergencies outside of your immediate surroundings allows you to be a responsible and compassionate member of your community. Enrolling in CPR training instills a sense of confidence in your ability to make a difference in the community. You become part of a network of individuals trained to respond effectively in life-threatening situations. By taking action and providing immediate CPR, you contribute to the well-being and safety of those around you. Your willingness to step up and help can inspire others to do the same, creating a culture of preparedness and compassion within the community.
- Contributing to a safer and more prepared society
CPR training plays a vital role in building a safer and more prepared society. The more individuals who are trained in CPR, the higher the chances of someone receiving immediate assistance in an emergency. By enrolling in CPR training, you contribute to the collective effort of ensuring the well-being and safety of society as a whole. By enrolling in CPR training, you become part of a network of individuals who are dedicated to saving lives. This network extends beyond your immediate circle of family and friends. You join a community of trained individuals who are ready to respond to emergencies and provide critical assistance. Together, you form a powerful force that can make a significant impact on the well-being and survival rates of those in need.
Factors to consider when choosing a CPR training program
- Accreditation and certification validity
Ensure that the CPR training program you choose is accredited by a recognized organization. Certification from reputable organizations such as the American Heart Association (AHA) holds more weight and validity. Check the certification requirements of your workplace or industry to ensure that the training program meets its standards.
- Course content and hands-on practice opportunities
Review the course content to ensure that it covers the necessary CPR techniques and procedures. Hands-on practice opportunities are crucial for mastering the skills required for CPR. Look for programs that offer ample time for practical exercises and simulations to enhance your confidence and proficiency.
- Cost and scheduling options
Consider the cost and scheduling options of the CPR training program. Compare prices and check if financial assistance or discounts are available. Additionally, check if the program offers flexible scheduling options to accommodate your needs. Enrolling in CPR training is a decision that can have a profound impact on your life and the lives of those around you. It equips you with the knowledge and skills needed to respond effectively in life-threatening situations, potentially saving lives. The benefits of CPR training are far-reaching, from ensuring the safety of your loved ones to being a valuable asset in the workplace, empowering yourself to take action in public settings, and contributing to a safer and more prepared society. CPR training is more than just a certification. It is a commitment to being prepared, taking action, and making a difference in critical moments. By enrolling in a CPR training program, you are equipping yourself with the tools to save lives and create a safer environment for yourself, your loved ones, and your community. The confidence and skills gained through CPR training are invaluable assets that can have a lasting impact. Remember, it only takes one person to make a difference, and that person could be you. Enroll in CPR training and become a lifesaver in your community. Together, let’s create a world where everyone is prepared to save a life. Looking for CPR training in Tampa? Join our BLS class in Tampa and gain essential life-saving skills. Enroll in our CPR class Tampa today and become equipped to handle emergencies with confidence. Trust our CPR Tampa training company to provide expert instruction and ensure you’re prepared to respond effectively in critical situations.



[grw id=”11782″]
Basic Life Support Training for Healthcare Professionals in Tampa: A Comprehensive Guide
 Basic Life Support (BLS) is a critical set of skills that every healthcare professional should possess. In emergency situations, BLS can mean the difference between life and death for patients. This article will provide an overview of BLS training, emphasizing its significance, and identifying those who should become certified in BLS. If you’re in Tampa and seeking to complete your BLS certification, CPR Tampa has you covered. Basic Life Support refers to the immediate medical care provided to individuals experiencing life-threatening emergencies. It focuses on maintaining and restoring proper circulation, establishing an open airway, ensuring proper breathing, and restoring circulation. BLS techniques are designed to be straightforward and easy to learn, enabling healthcare professionals to administer timely assistance until advanced medical support arrives. Healthcare professionals are often the first responders in emergency situations, and their knowledge and proficiency in BLS can make a substantial difference in patient outcomes. BLS training equips healthcare providers with the necessary skills and confidence to handle critical situations effectively, potentially saving lives. Basic Life Support training is beneficial for a wide range of healthcare professionals, including doctors, nurses, emergency medical technicians (EMTs), paramedics, dentists, and pharmacists. Whether you work in a hospital, clinic, or any other healthcare setting, BLS training should be a priority to ensure you are prepared to handle emergencies effectively.
Basic Life Support (BLS) is a critical set of skills that every healthcare professional should possess. In emergency situations, BLS can mean the difference between life and death for patients. This article will provide an overview of BLS training, emphasizing its significance, and identifying those who should become certified in BLS. If you’re in Tampa and seeking to complete your BLS certification, CPR Tampa has you covered. Basic Life Support refers to the immediate medical care provided to individuals experiencing life-threatening emergencies. It focuses on maintaining and restoring proper circulation, establishing an open airway, ensuring proper breathing, and restoring circulation. BLS techniques are designed to be straightforward and easy to learn, enabling healthcare professionals to administer timely assistance until advanced medical support arrives. Healthcare professionals are often the first responders in emergency situations, and their knowledge and proficiency in BLS can make a substantial difference in patient outcomes. BLS training equips healthcare providers with the necessary skills and confidence to handle critical situations effectively, potentially saving lives. Basic Life Support training is beneficial for a wide range of healthcare professionals, including doctors, nurses, emergency medical technicians (EMTs), paramedics, dentists, and pharmacists. Whether you work in a hospital, clinic, or any other healthcare setting, BLS training should be a priority to ensure you are prepared to handle emergencies effectively.
The CABs of Basic Life Support
Understanding the fundamental aspects of BLS is crucial for healthcare professionals. Let’s explore the three main components of BLS: Compressions, Airway, and Breathing. Compressions: Compressions keep oxygenated blood moving throughout the body. In BLS, healthcare professionals learn techniques such as chest compressions and the proper use of automated external defibrillators (AEDs) to maintain and restore circulation. Airway: The next step in BLS is to ensure an open airway. This involves assessing the patient’s airway, clearing any obstructions, and positioning them appropriately to maintain an unobstructed passage for breathing. Breathing: The next focus is on assessing breathing patterns and providing rescue breaths if necessary. Healthcare professionals should be familiar with various techniques, such as mouth-to-mouth resuscitation, the use of barrier devices, or bag-mask devices to provide adequate ventilation.
AED
An Automated External Defibrillator (AED) is a portable device used to analyze a person’s heart rhythm and deliver an electric shock, if required, to restore a normal heartbeat. AEDs are critical in cases of sudden cardiac arrest, as they can significantly increase the chances of survival. Let’s take a closer look at the functions and significance of AEDs. Understanding their purpose is essential for healthcare professionals to effectively utilize these life-saving devices. Learning to operate an AED is an integral part of BLS training. The BLS course will provide hands-on instruction for applying pads, operating the device, and following the prompts provided by the AED. Simulations and practical exercises help healthcare professionals gain confidence in utilizing AEDs during emergencies. Knowing when to use an AED is equally vital. BLS training covers the recognition of cardiac arrest symptoms and the appropriate steps to take in activating an AED. Understanding the proper timing for AED deployment can significantly increase the chances of a positive outcome for the patient.
CPR
Cardiopulmonary Resuscitation (CPR) is a core component of BLS training. CPR involves a combination of chest compressions and rescue breaths to maintain blood flow and oxygenation in individuals experiencing cardiac arrest or respiratory failure. Let’s explore the steps involved in performing CPR on different age groups.
How to perform CPR on an infant
When performing CPR on an infant, healthcare professionals should follow specific guidelines tailored to their size and needs. The course will cover techniques such as providing gentle chest compressions with two fingers, ensuring proper head positioning, and delivering delicate rescue breaths.
How to perform CPR on a child
CPR techniques for children are slightly different from those used for infants and adults. Healthcare professionals will learn to adapt their approach by providing chest compressions with the heel of one hand, ensuring an open airway, and delivering effective rescue breaths.
How to perform CPR on an adult
CPR for adults follows a similar approach to child CPR but with some modifications. The course will cover techniques such as providing chest compressions with the heel of both hands, positioning the patient correctly, and ensuring effective ventilation during rescue breaths.
Basic Life Support Skills
To reinforce the skills learned during BLS training, hands-on practice sessions are crucial. These practice sessions provide an opportunity for healthcare professionals to refine their techniques, build muscle memory, and gain confidence in their abilities. Here are some essential components of BLS skills practice:
- Hands-on practice of adult and pediatric CPR techniques: Participants will practice performing chest compressions, rescue breaths, and the proper ratio of compressions to breaths for both adults and pediatric patients.
- Demonstration and practice of AED use: Participants will receive instruction on AED operation and have the chance to practice using the device in simulated scenarios. This practical experience helps healthcare professionals become familiar with AED prompts and gain confidence in their ability to utilize this life-saving equipment.
- Simulation-based scenarios for team coordination and communication: BLS training often incorporates simulated scenarios that mimic real-life emergency situations. These scenarios encourage participants to work as a team, communicate effectively, and make critical decisions under pressure. This interactive approach enhances readiness and prepares healthcare professionals for the challenges they may face in the field.
Basic Life Support training is a vital component of healthcare professionals’ skill set, ensuring they can effectively respond to life-threatening emergencies. By prioritizing BLS training and honing these life-saving skills, healthcare professionals can enhance their ability to save lives and provide immediate care in critical situations. Attention healthcare professionals in Tampa! Are you equipped with the vital skills needed to save lives in critical situations? Look no further than our comprehensive Basic Life Support (BLS) training program, tailored specifically for healthcare professionals like you. Our expert instructors will guide you through hands-on CPR Tampa sessions, empowering you with the knowledge and confidence to respond effectively in emergencies. Don’t miss this opportunity to enhance your skills and become a valuable asset to your patients and community. Register now for our BLS Tampa course and take the first step towards saving lives with confidence.



[grw id=”11782″]
Header Content
What is Chronic Kidney Disease by Samiya Tazeen
There are a few risk factors that might increase an individual’s risk of getting chronic kidney disease. Some of the factors are smoking, heart disease, obesity, cholesterol, family history of kidney disease, seniors, and being an African –American, Native American, or Asian- American. People that have chronic kidney disease have a higher risk of getting heart and blood vessel disease. Not many symptoms might appear or be severe until the kidney disease is chronic. But, some of the symptoms that might be noticeable are fatigue, trouble sleeping, swelling of feet and ankles, hypertension (high blood pressure), and itchiness. People that have chronic kidney disease can have many complications that could affect their body. Some of the complications might include fluid retention, rise in potassium levels which might decrease the function of your heart, heart disease, damage to central nervous system, increased risk of getting an infection, end-stage kidney disease, anemia (low blood count), and pericarditis (an inflammation of the pericardium).
Unfortunately, there is no cure for chronic kidney disease. The treatment for chronic kidney disease is to reduce complications, and slow the progress of the disease. Treatment for chronic kidney disease depends on the cause of the disease. Even if the cause is controlled, kidney disease might continue to progress and get worse. For example, if the sugar level of a person that has diabetes is controlled his/her kidney disease still might continue to worsen. Many of the medications that are given to people that have kidney disease are to reduce a complication. Some of the medications that are given to those suffering are medications that lower high blood pressure, medications that lower cholesterol levels, medications that increase your blood count/treat anemia, medications that reduce fluid retention (swelling of legs), and medications that protect your bones.
When a person completes kidney failure or are near a kidney failure, then they have end-stage kidney disease. At end-stage kidney disease, a person needs dialysis or a kidney transplant. Dialysis artificially removes waste products and fluids from the blood. There are two types of dialysis: hemodialysis, and peritoneal dialysis. In hemodialysis, a machine filters waste products and fluids from your blood. In peritoneal dialysis, the inside lining of the abdomen acts a filter and wastes are taken out by a solution. In a kidney transplant, a healthy kidney from a donor is placed into the patient’s body surgically. Kidneys can be transplanted from a deceased donor or a living donor. After the kidney is transplanted, the person needs to take medications for the rest of his/her life to keep the body from rejecting the kidney.
A person that has an increased risk of getting chronic kidney disease can determine if they have kidney disease from the following tests. Blood tests can determine the creatinine and urea in the blood, which determines the level of waste in the blood. The second test is a urine test. A urine test can help identify the causes of the kidney disease. Glomerular Filtration Rate (GFR) is the best test to measure the level of kidney function. An ultra sound or CT scan can also help tell whether the kidneys are too small or large, and if a person has any kidney stones.
References:
National Kidney Foundation
MayoClinic






What is Macular Degeneration by Lilli Goldman
Imagine a hole in the center of your vision, one you can’t look over or under, to the left or to the right of. A central vision obstruction like this is one of the salient characteristics of Macular Degeneration, a common cause of vision loss for persons over age 50.
It results from damage to the macula–the center of the eye’s retina, which is needed for clear straight ahead vision. Millions of light sensors in these most sensitive areas of the retina at the back of the eye are needed to send electronic signals through the optic nurse to the brain, where images are translated into a navigable world.
The advance of the disease is slow in most cases, but can occur quickly. It can occur in one or both eyes, beginning with a blurred center of vision, a loss of overall brightness and a blank spot. The center field of vision is dark, distorted and blurry. When it occurs in just one eye, as is often the case, the other eye compensates so that the person may not be aware of a loss of vision. This is why routine eye exams are necessary, especially in individuals over age 50.
Macular Degeneration results in hampered vision, and not usually in complete blindness unless other complicating factors are in play. But even so, the results of Macular Degeneration can be life shattering. Reading, writing, cooking, recognition of faces, and any close work will be difficult to the point of impossible. A person’s daily activities will have to be wholly altered to adapt to the new visual limitations.
To avoid Macular Degeneration, older individuals should have routine eye exams and in addition should manage any other diseases. Smoking is harmful to the eyes, and is a known risk factor. It doubles the risk of Macular Degeneration. People should stay at a healthy weight to lessen their chances of Macular Degeneration. Further, they should exercise regularly, as we all should for many reasons. A nutritious diet featuring fruits, leafy green vegetables and fish should be adopted.
A study from the National Health Association (NHANES) and published in the Journal of American Geriatrics examined the effect of wine drinking on Macular Degeneration. The lowest risk seemed to be for persons drinking one glass of wine per month. Beer and liquor seemed to have no effect. The study has since been questioned (American Macular Degeneration Foundation, 1998).
Zeaxanthin, an ingredient found in corn, spinach, collards, orange juice, lettuce, oranges, tangerines, and peas (in that order of decreasing strengths) seems helpful. High doses of certain vitamins may also be helpful, as formulated by the National Eye care Institute (2005).
| Vitamin C | 500 mg |
| Vitamin E | 400 mg |
| Zinc | 80 mg |
| Copper | 2 mg |
| Beta Carotene or lutein or Zeaxanthin | 15 mg |
Other known risk factors include ethnicity: Caucasians have a higher rate than African American or Hispanics. A family history of Macular Degeneration is also a risk factor as genetics seem to predispose persons to the condition.
Lifestyle factors other than avoidance of smoking include a close monitor of blood pressure, an exercise regimen and a diet of fish and green, leafy vegetables.
Detection of Macular Degeneration begins with a visual acuity test which checks for distances in vision. A Dilated Exam follows in which drops for the back of the eye allow a view with the use of a magnifier. Amster Grid tests are used to show the extent of the loss, and Fluorescein angiograms look for leaks in the arteries of the eye, using a dye injected in the arm of a patient. Optical coherence tomography is also used, with light waves providing a painless detection test.
The eye care professions are looking for drusen, a yellow deposit that accompanies the aging process. Another sign is pigment changes under the retina. Dark clumps of released pigment are seen, which do not affect the eye color, but surround the retina from underneath.
In the early stages of Macular Degeneration, the drusen is the width of a hair and no vision loss is yet reported.
In the intermediate state large drusen is seen, with some vision loss.
In the late stages, geographic atrophy, or dry Macular Degeneration is having a gradual breakdown. With neovascular Macular Degeneration, or wet, the blood vessels under the retina are seen to leak fluid and blood. Swelling and damage to the eye is occurring.
The early stages show few symptoms, and not all Macular Degeneration will develop. If it is in one eye only, only 5% of persons will get advanced Macular Degeneration in 10 years. With both eyes affected, 14% will get advances stages in 10 years (National Eye care Institute, 2014).
Treatment is not required for early states. Lifestyle changes may help and be recommended. With Intermediate stages high dosage vitamins may be prescribed.
In advanced stages, injections of anti vascular endothelial growth factor may be done the multiple monthly injections. The eye is numbed and cleaned first. The injections are made and antibiotic drops are prescribed afterwards.
Photo dynamic therapy laser treatments may be used with a drug injected in the arm, to allow the laser to close vessels in the eye. This procedure is less common and mostly used in combination with other treatments.
Macular Degeneration strikes fear in patients and their loved ones. It is a diagnosis one never wants to hear, but it does not predict total blindness. It can be slow in advancing, compensated for, or treated. As with any unfavorable diagnosis, support groups can be helpful. Low vision adjustments such as reading glasses, magnifying glasses, and other accouterments can help persons find normalcy in the midst of visual limitations.
References
Mayo Clinic, “Dry macular degeneration,” http://www.mayoclinic.org/diseases-conditions/macular-degeneration/basics/prevention/con-20075882 accessed May 3, 2015.
American Macular Degeneration Foundation, http://www.afb.org/directory/profile/american-macular-degeneration-foundation/12 accessed May 3, 1015.







How Do You Treat Tuberculosis by Ammara Semeen
Tuberculosis can also be caused by close contacts of a person with contagious TB disease. Persons who have emigrated from different parts of the world with high TB rates can also get infected. Children who are less than five years of age who had a positive TB test can also have chances of getting infected with TB again. Persons with weak immune system or people who had any of the diseases or conditions like HIV infection, Substance abuse, Low body weight, kidney diseases, organ transplants or Diabetes mellitus also have chances of getting Tuberculosis in their life.
The symptoms of Tuberculosis include coughing with blood, which can lasts 3 weeks or longer, pain in the chest, weight loss weakness, heavy fever, chills and sweating at night. Latent TB infection does not have any symptoms and they cannot spread TB bacteria. If you have a relative or a friend who has been exposed to TB then you should contact a doctor and get tested to make sure you didn’t get exposed to TB as well. There are two types of tests that are used to detect TB bacteria. Tuberculin skin test (TST), which is done by injecting a fluid, called as tuberculin. The fluid is injected in the lower part of the arm. The person who is given this test has to wait for 48 to 72 hours and then returns to get the arm checked. The doctor or health care worker will look at the hand and if the hand area is swelled then using a ruler it is measured. TB blood test also known as interferon-gamma release assays (IGRAS) measures how the immune system reacts to the TB bacteria by testing the person’s blood. A positive IGRA test means that the person has been infected with Tuberculosis and treatment for TB is needed. A negative IGRA test means the person’s blood did not reacted to the test and the person does not have TB disease.
Latent TB infection is treated by medications such as isoniazid (INH), rifampin (RIF), rifapentine (RPT). Taking medications for 6 to 9 months treats TB disease. The medications for TB disease include isoniazid (INH), rifampin (RIF), ethambutol (EMB), and pyrazinamide (PZA). If the person infected with TB stops taking the medicine too soon then they can become sick again and the TB may become active. Sometimes people can become resistance to the TB drugs, which means the medications used for treating TB can no longer kill the bacteria in the person. Drug Resistant to TB can occur if people do not take the medications regularly or if they do not take all of their drugs. If the qualities of the drugs are poor or if the health care provider prescribes the wrong medication with wrong dose or the length of time for taking the drugs in shortened then they the medications will not affect the person and it can’t kill the bacteria in the body. To prevent the spread of drug –resistant TB then the person should take all the medications exactly as prescribed. The treatment should not be stopped early as the TB bacteria are still present in the body and they can get infected with Tuberculosis again.
References:
http://www.webmd.com/a-to-z-guides/understanding-tuberculosis-basics







Discussion Section | Microbiology Unknown Report, Pseudomonas aeruginosa
DISCUSSION/CONCLUSION:
How did the test results lead to the identification?
Different bacteria can live and flourish in certain environments, while others will die or never grow in the very same environment due to their dissimilar characteristics. These tests help determine which bacteria can grow in certain situations. For both bacteria, the Gram stain was a necessity in order to determine if the microbe was Gram Positive or Gram Negative. Once the Gram Positive bacteria was successfully visible under the microscope, it was clear that it was cocci. Knowing this information helped to cross two bacteria (both rods) off the unknown list. From there, the Mannitol test helped narrow down the choices even more. This particular Gram Positive microbe was able to ferment Mannitol and produce acid giving it a positive result. This positive result narrowed the choices down from three to two (S. aureus and E. faecalis). The only test that would allow for differentiation between these two bacteria was the Nitrate reduction test. This test came back negative, which meant this microbe could not reduce nitrate to nitrite or any other nitrogenous compounds. Only one Gram Positive bacteria given cannot reduce nitrate, which lead to its identification: E. faecalis.
The other Gram stained slide was viewed under the microscopes and pink/reddish rods were clearly visible making it the Gram negative bacteria. This Gram stain, however, did not eliminate any of the Gram Negative bacteria because they were all rods. The first test was the Simmons Citrate test. This test determines whether or not a microbe can use citrate as its sole carbon source. It was a positive result, meaning it could in fact use citrate as its only carbon source. This test narrowed down the choices from five to three bacteria (K. pneumoniae, E. aerogenes, and P. aeruginosa). The Urea test was then conducted. This test is used to identify bacteria capable of hydrolyzing urea using the enzyme urease. The test came back negative, which helped to eliminate K. pneumoniae, since that particular bacteria produces urease. Casein was the last test used in order to identify the Gram Negative bacteria. After incubation, there was a clearing in the milk agar, which proved that this bacteria could hydrolyze the milk protein casein using the enzyme casease. The only bacteria that was able to do that was P. aeruginosa.
Was it the correct identification?
After showing the professor the results that lead to the identification of these bacteria (E. faecalis and P. aeruginosa), it was confirmed the correct microbes were found.
What problems were encountered?
The only problem that was encountered was during the original streak plate. After two days of incubation, it was hard to isolate two different bacteria into two separate nutrient agar plates due to overgrowth. In order to avoid contamination or future problems, another streak plate was done and more carefully. After the second try, two separate bacteria were growing and it was possible to successfully isolate them both.
Pseudomonas aeruginosa
Pseudomonas aeruginosa wasn’t successfully isolated until 1882. In a publication entitled when “On the Blue and Green Coloration of Bandages”, Carle Gessard reported the growth of the organism from cutaneous wounds of two patients with bluish-green pus (3). P. aeruginosa is a gram negative, rod shaped bacteria. It is a strictly aerobic microbe, which means it needs oxygen to grow and survive. It is noted for its ability to live in versatile environments, cause nosocomial infections in susceptible individuals and it’s resistance against antibiotics.
P. aeruginosa is an important microbe to be aware of because it has an ability to survive with minimal nutrients and can tolerate a variety of physical conditions. This allows P. aeruginosa to be prevalent in both hospital settings, as well as, in our overall community. While in the hospital, P. aeruginosa can be found on a variety of equipment. Such equipment includes: respiratory machines, antiseptics, soaps, mops, etc. (3). While out in the community, P. aeruginosa can be found in swimming pools, hot tubs, humidifiers, and even vegetables. While P. aeruginosa is still prevalent in our community, it is in hospitals that this bacteria can cause major infection. It is considered an opportunistic pathogen, which means it usually does not pose a problem, however, it can become pathogenic. When a person enters a hospital, it is normal for their immune system to be compromised. When an individual becomes immunocompromised their ability to fight off an opportunistic pathogen like P. aeruginosa becomes more difficult.
While P. aeruginosa normally does not cause illness in a healthy person, it can cause major problems for an individual in the hospital with a compromised immune system. It is the most common pathogen isolated from patients who have been hospitalized longer than 1 week (4). Some common nosocomial infections caused by P. aeruginosa include: pneumonia, urinary tract infections, blood stream infections, as well as, infection of surgical sites. Nosocomial P. aeruginosa infections can be dangerous because the individual is already under either physical or mental stress (or both), but another frightening fact is that P. aeruginosa is resistant to many antibiotics.
P. aeruginosa can develop resistance to antibiotics, either through the acquisition of resistance genes on mobile genetic elements (i.e., plasmids) or through mutational processes that alter the expression and/or function of chromosomally encoded mechanisms. (3) While these drug resistant abilities are positive aspects for P. aeruginosa, it is very dangerous for individuals fighting infection. The drug resistance makes treating this pathogen even more difficult and vastly limits avenues in which doctors can take to help treat patients with this infection. The question then becomes, if there is an overuse of the antibiotics that do work, will P. aeruginosa become resistant to those too?
REFERENCES:
(1) McDonald, Virginia (et al.). Lab Manuel for General Microbiology. Saint Louis Community College
at Meramec. 2011
(2) Lab Review for Practical Microbiology.
(3) Lister, Philip D. (et al). “Antibacterial-Resistant Pseudomonas aeruginosa: Clinical Impact and
Complex Regulation of Chromosomally Encoded Resistance Mechanisms.”
www.ncbi.nlm.gov/pmc/articles. American Society of Microbiology. 2009. April 28, 2015.
(4) Lessnau, Dieter-Klaus, MD. “Pseudomonas aeruginosa Infections.”
www.emedicine.medscape.com/article/226748. WebMD LLC. 2014. April 28, 2015.







What is Aortic Valve Stenosis by Madison Baysinger
Aortic valve stenosis (also called aortic stenosis or AS) is a condition where the heart’s aortic value has narrowed. This narrowing causes blood flowing from the left ventricle to the aorta and arteries to be impeded. It is estimated that up to 1.5 million people in the United States- with 500,000 of those being severe cases of AS. Aortic stenosis in some cases can lead to heart failure and sudden death.
There are three known causes of AS- progressive congenital wear and tear of a bicuspid valve, deterioration of the aortic valve in elderly people, and scarring of the aortic valve caused by rheumatic fever as a young adult or child. A bicuspid valve is the most common cause of AS. Because there is only two cusps instead of the usual three they cannot open as widely and blood flow is less controlled, the lack of control leads to more wear and tear on the leaflets. The increased wear and tear leads to scarring, lessened mobility, and calcification of the valve leaflets. In patients over age 65, protein collagen in the leaflets is lost and calcium deposits on them, this is called “senile calcific aortic stenosis.” When the mobility of the leaflets is decreased by calcium it causes thickening and scarring occurs, leading to AS. Unlike other heart conditions related to calcium deposits, this isn’t increased by unhealthy lifestyle choices. The third cause of aortic stenosis is damage from rheumatic fever. Rheumatic fever, caused by streptococcal bacteria, damages the valve leaflets themselves by making the edges of the leaflets fuse together. Rheumatic aortic stenosis is uncommon in the United States.
Common symptoms of aortic stenosis are chest pain, breathlessness, fainting, and palpitations. In rare cases the first and only symptom is sudden death. One-third of patients experience chest pain first, and over 50 percent report it as the condition progresses. This chest pain is caused by the higher pressure needed to pump blood through the damaged aortic valve and oxygen demand of the thickened muscle. During excitement and exercise, fainting can be a symptom of AS because of vasodilation leading to lowered blood pressure. With the damaged aortic valve the heart has trouble keeping up with the blood pressure drop, leading the patient to faint. It is believed that after the onset of chest pain and fainting life expectancy is less than three years without treatment. Shortness of breath due to heart failure is thought to be the most worrying sign of aortic stenosis. During the beginning of the condition it only happens during high levels of activity and decreases when resting. In later stages of aortic valve stenosis shortness of breath can even happen during rest, especially when lying flat. Life expectancy is only 6 to 24 months after this sets in.
Aortic valve stenosis is diagnosed and evaluated in four ways. An electrocardiogram can show odd arrangement of the heart’s electrical activity, which may reveal thickened muscle of the heart and lead to a diagnosis. An echocardiography obtains images of heart chambers and valves, showing the damaged valve. Thirdly, using a chest x-ray shows a dilated aortic valve. The most reputable method of diagnosing AS is cardiac catheterization. This measures the pressure on both sides of the valve and that can be used to determine valve area.
Treatment of aortic stenosis depends on the severity of the condition. In cases where the patient experiences little to no symptoms, a doctor will only monitor because surgery would be riskier than the condition itself. In mild cases, or with patients who aren’t able to receive surgery, balloon valvuloplasty can temporarily relieve AS. If severe AS is found, aortic valve replacement, either mechanical or bio-prostheses (from pigs or cows) is the usual treatment.
As with many diseases, the most important thing for patients with aortic valve stenosis is careful monitoring. Many people with this condition can live to fulfilling lives. Research continues to improve lives of the people diagnosed with this disease and increase life expectancy of patients.
References:
http://www.mayoclinic.org/diseases-conditions/aortic-stenosis/basics/definition/con-20026329 (Mayo Clinic)
http://www.medicinenet.com/aortic_stenosis/page4.htm (Medicine Net)
http://www.heart.org/HEARTORG/Conditions/More/HeartValveProblemsandDisease/Problem-Aortic-Valve-Stenosis_UCM_450437_Article.jsp (American Heart Association)
http://www.webmd.com/heart-disease/tc/aortic-valve-stenosis-overview (WedMD)







Identifying Staphylococcus aureus | Microbiology Unknown Lab
UNKNOWN LAB REPORT
Unknown Number 120, Alternate 3
Emily Specter
May 5, 2015
Professor Jay Snaric
Introduction to Microbiology
Spring 2015
INTRODUCTION
Although naked to the eye, microorganisms play a key role in the lives of every human being. In the health field, while microorganisms are responsible for causing diseases, they are also actively involved in the making of antibiotics. Without identifying the microorganisms that caused the disease, it would be impossible to isolate an antibiotic that would successfully treat the patient. Similarly, in the food business, microorganisms are involved in managing food safety and maintaining a high quality of food. In this scenario, it is vital that the correct bacteria are identified and used when cooking and keeping supplies and utensils free of harmful microorganisms. This study involves utilizing all of the methods and procedures covered in the microbiology laboratory class in order to learn the process of correctly identifying the two unknown bacteria.
MATERIALS AND METHODS
At the beginning, a test tube labeled 120 was handed out by the lab instructor. In order to isolate the two unknown bacteria from the single test tube, an isolation streak plate needed to be performed. This procedure, as outlined in the lab manual written by McDonald et al., carefully pulls bacteria along the four sides of a nutrient agar plate to try to clearly isolate the two microbes (10). After forty-eight hours of incubation at thirty-seven degrees Celsius, it appeared as if only one type of bacterium grew on the streak plate. Although only one bacterium had grown, it was in the best interest of the study to keep working, and then return to the other bacterium once it had been determined whether it was gram positive or gram negative. Moving forward, another isolation streak plate was performed using just the one bacterium that appeared on the original streak plate. Once incubated, the nutrient agar came back pure, thus allowing a procedure called a gram stain to be performed. Described in the lab manual by McDonald et al., the gram stain was performed using the microbes from the inoculated agar plate and came back as gram positive cocci (67). Then, a urea test and a nitrate test were both performed on the gram positive cocci. The urea test requires urea broth tubes, while the nitrate test requires nitrate broth tubes, nitrate reagent A, nitrate reagent B, and powdered zinc. Both tests are further outlined in the laboratory manual (McDonald et al. 36). Once these tests were completed, the identity of the unknown bacterium was revealed.
Gram Positive Methods
| TEST | PURPOSE | REAGENTS | OBSERVATIONS | RESULTS |
| Gram Stain | To differentiate bacterial cells based on their cell wall | Crystal violet, Iodine, Alcohol, Safranin | Purple balls | Gram Positive cocci |
| Urea Test | To determine if bacteria had made urease, thus broke down urea | None | Urea broth remained tan color (unchanged) | Negative Result |
| Nitrate Test | Tests for the reduction of nitrate | Nitrate Reagent A, Nitrate Reagent B, Powdered zinc | Add reagents, No color change, added zinc, no color change | Positive Result |
When isolating the bacteria at the very beginning on the isolation streak plates, only the gram positive bacterium was visible. At this point in the study, the gram negative bacteria were needed to grow, so EMB agar and MacConkey agar were chosen to be inoculated. These specific agars were chosen because they inhibit the growth of gram positive bacteria and select for the growth of gram negative bacteria. After incubation, there were visible purple spots on the EMB agar so a gram stain was performed with those microbes and gram negative and gram positive bacteria appeared. Due to this, the lab instructor handed out an alternate number three. Using the alternate number three, a nutrient agar plate was streaked, incubated, and then gram stained. The gram stain confirmed that alternate number three was gram negative rods. Then, a urea test, a sulfur reduction test, and an indole test were performed. The urea test requires urea broth tubes, the sulfur reduction test requires a SIM tube, and an indole test requires a SIM tube and indole reagent. All three of these tests are described in the laboratory manual (McDonald et al. 19,36). The results of these tests confirmed the identity of the second unknown bacterium.
Gram Negative Methods
| TEST | PURPOSE | REAGENTS | OBSERVATIONS | RESULTS |
| Gram Stain | To differentiate bacterial cells based on their cell wall | Crystal violet, Iodine, Alcohol, Safranin | Pink rods | Gram negative Rods |
| Urea Test | To determine if bacteria had made urease, thus broke down urea | None | Urea broth turned bright pink | Positive result |
| H2S Test | To determine if sulfur had been reduced | None | Tube had a black clump | Positive result |
| Indole Test | To determine if indole had been produced | Indole reagent | Top of test tube appeared red | Positive result |
RESULTS
Starting with the first unknown, a gram stain, urea test, and nitrate test were performed. The gram stain revealed that the unknown was a gram positive cocci bacterium. In addition, the urea test was negative and the nitrate test was positive. The second unknown was a gram negative rod and that bacterium had three separate tests performed. Specifically, the urea test was positive, the H2S test was positive, and the indole test was positive. In conclusion, the gram positive bacterium was Staphylococcus aureus, and the gram negative bacterium was Proteus vulgaris.
Biochemical Tests – Gram Positive
| TEST | REAGENTS/MEDIA | TEMP | OBSERVATIONS | RESULTS | INTERPRETATIONS |
| Gram Stain | Crystal violet, iodine, alcohol, safranin | 23OC(room temp) | Purple balls | Gram positive cocci | Organism has cell walls made of thick peptidoglycan |
| Urea | Urea broth | 37OC | Urea broth remained tan colored (unchanged) | Negative result | Bacteria do not produce urease, so urea is not broken down |
| Nitrate | Nitrate broth, nitrate reagent A, nitrate reagent B, powdered zinc | 37OC | Add reagents, no color change, added zinc, no color change | Positive result | Nitrate has been fully reduced |
Biochemical Tests – Gram Negative
| TEST | REAGENTS/MEDIA | TEMP | OBSERVATIONS | RESULTS | INTERPRETATIONS |
| Gram stain | Crystal violet, iodine, alcohol, safranin | 23OC(room temp) | Pink rods | Gram negative rods | Organism has a thinner layer of peptidoglycan and an outer lipid membrane |
| Urea | Urea broth | 37OC | Urea broth turned bright pink | Positive result | Urea is broken down by urease |
| H2S | SIM tube | 37OC | Black clump appeared in tube | Positive result | Organism produces hydrogen sulfide |
| Indole | SIM tube, indole reagent | 37OC | Top of test tube appeared red | Positive result | Organism produces indole and is a bi-product of amino acid metabolism |
FLOW CHART – Removed due to formatting issues.
DISCUSSION/CONCLUSION
Through multiple tests and procedures, the identity of both unknowns were determined. Once the gram stain revealed that the gram positive bacterium was cocci, the bacteria Bacillus cereus and Bacillus subtillis could be excluded because they are rod shaped. The first test performed for the gram positive bacteria was the urea test. This test yielded negative results and thus eliminated Staphylococcus epidermidis. Then, the nitrate test confirmed that Enterococcus faecalis was not the unknown, and rather Staphylococcus aureus was.
When the urea test was performed on the gram negative bacteria, the results were positive, which eliminated the bacteria Escherichia coli, Enterobacter aerogenes, and Pseudomonas aeruginosa. Next, the sulfur reduction test determined that the unknown is not Klebsiella pneumoniae, leaving only one option, which is Proteus vulgaris. The indole test also confirms that the unknown bacterium is Proteus vulgaris.
All of these tests executed led to the correct identities of both unknowns. The only problem that was encountered throughout the process, was when the gram stain was performed using the bacteria from the EMB agar and both gram negative and gram positive bacteria grew. Using the EMB agar, only gram negative bacteria was supposed to grow, but because both types of bacteria grew, an alternate bacteria was given by the instructor.
Staphylococcus aureus is a gram positive, facultative anaerobic bacteria. It is normally found in the nose and on the skin of 25%-30% of healthy adults and 25% of people in the hospital [“Staph Infection (Staphylococcus aureus)”]. Usually, this bacteria is not harmful when it is outside the body; however, once the bacteria enters the body, disease and infection follows. While skin infections are most commonly caused by S. aureus, this bacteria can also cause pneumonia, food poisoning, toxic shock syndrome, and blood poisoning (“Staphylococcal”). Some symptoms and signs of a localized staph infection include pus, tenderness, pain, redness, swelling, and drainage. In specific cases, staph infections are contagious until they are resolved. Infections could be spread through personal hygiene items like razors and bandages. Certain people, such as newborns, breastfeeding women, and people with chronic conditions such as diabetes, cancer, vascular disease, lung disease, and weakened immune system, are at a greater risk of infection. Depending on the type of staph infection, there are different modes of treatment. Minor skin infections may be treated with antibiotic ointment, while other staph infections may be treated with oral, or IV antibiotics [“Staph Infection (Staphylococcus aureus)”].
Staphylococcus aureus can also cause food poisoning if food is not refrigerated properly or if someone accidently contaminates the food. The incubation period is one to six hours and the symptoms may include nausea, vomiting, diarrhea, loss of appetite, severe abdominal cramps, and fever. Typically, the food poisoning lasts twenty-four to fourty-eight hours. Steps such as washing hands before handling food, keeping kitchens and serving areas sanitized, and avoiding handling food if you have an infection or cut can be taken to prevent food poisoning (United).
Methicillin resistant Staphylococcus aureus (also known as MRSA) is a strain of bacteria that is resistant to antibiotics that are usually used to treat staph infections. There are two main forms, one that is health-care associated, and one that is community associated. MRSA is more difficult to treat than typical staph infections and can affect the bloodstream, lungs, heart, bones, and joints [“Staph Infection (Staphylococcus aureus)”].
There are several ways to reduce one’s risk of developing a staph infection. First and foremost, washing hands with soap and water helps defend against germs and Staphylococcus aureus. Also, one should keep wounds covered and avoid sharing personal items such as razors and towels. For women, it is important to change tampons frequently because S. aureus can cause toxic shock syndrome if tampons are left in for extended periods of time. Lastly, one should wash clothing and sheets in hot water to remove all bacteria (“Staph Infections” Mayo). Staphylococcus aureus is all around us, but with proper knowledge and awareness, disease and infection can be avoided.
Works Cited
McDonald, Virginia, Mary Thoele, Bill Salsgiver, and Susie Gero. Lab Manual for General Microbiology. Saint Louis:STLCC-Meramec, 2011. Print.
“Staph Infection (Staphylococcus Aureus).” Medicinenet.com. Medicinenet, Inc, 4 Mar. 2015. Web. 29 Apr. 2015.
“Staph Infections.” Mayo Clinic. Mayo Foundation, 11 June 2014. Web. 29 Apr. 2015.
“Staphylococcal Infections.” MedlinePlus. U.S. National Library of Medicine, 2 Oct. 2014. Web. 29 Apr. 2015.
United States. U.S. Dept. of Health and Human Services. “Staphylococcus.” Foodsafety.gov. n.d. Web. 30 Apr. 2015.








